PCOS test is based on the Rotterdam criteria for diagnosing PCOS.
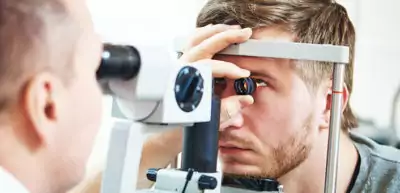
Arthritis
Most people associate joint pain and swelling as common symptoms of arthritis. This is true for one kind of arthritis, called osteoarthritis. However, other forms of arthritis such as rheumatoid arthritis and reactive arthritis may bring other surprising complications. Eye problems are an example.
According to estimates, about 30 to 40% of people living with rheumatoid arthritis will have eye problems of some kind. The most common problem is dryness, which can damage the cornea. Dryness can even lead to severe vision-threatening complications.
As a medical doctor, I get very concerned when people ignore eye complications as a serious risk of arthritis. Let me share some common eye complications of arthritis along with their symptoms & causes and steps to safeguard your eyes and prevent permanent damage.
Dry eye, medically known as keratitis sicca, is a condition where your eyes are unable to maintain adequate moisture in them. In other words, your eyes are unable to maintain healthy tear films, which not only lubricate the eyes but also protect them from foreign particles. Adequate moisture of eyes is also a key requirement for good vision.
People with dry eyes may experience itching or irritation, as if grains of sand are stuck in the eyes. Some folks also experience blurred vision. Symptoms may get worse with each passing day.
Dry eye syndrome is the most common eye problem in people with rheumatoid arthritis. It may also be associated with another autoimmune condition called Sjogren’s syndrome.
A test known as Schirmer’s test is used for diagnosing dry eye syndrome. In this test, a small paper strip is put inside the bottom lid of each eye. A doctor checks these strips at an interval of five minutes. The wetness of your strip will indicate whether your tear glands are functioning properly or not.
Although further studies are needed to prove the effectiveness of these methods, some alternative medicine approaches to deal with dry eye include:
Before using any form of alternative medicine, people with dry eyes should discuss the risks and benefits with a doctor.
If your symptoms are severe, your doctor might recommend tear substitutes. It is advisable to consult an ophthalmologist rather than going for over-the-counter eye drops, which may contain certain avoidable preservatives.
In case of very severe dry eyes, your doctor might prescribe cyclosporine drops, which are immunosuppressive in nature. The option of punctal plugs is also available wherein a small plug is inserted into the tear duct to prevent the eye from draining.
Flaxseed oil and fish oil contain important dietary fatty acids that have multiple health benefits, including prevention or treatment of dry eyes.
Daily supplements of flaxseed oil or fish oil, when used alone or in tandem with lubricating eye drops, can reduce the key symptoms of dry eye such as burning, stinging, redness and intermittent visual disturbances. For this reason, many eye doctors now are recommending flaxseed oil and fish oil supplements for dry eyes. Additionally, omega 3 fats, found in fish oil have the benefit of reducing overall systemic inflammation. People with rheumatoid arthritis often find joint pain relief with omega 3 supplements for this reason.
There is limited evidence that vitamin supplementation helps in the treatment of dry eyes. Also, there is insufficient evidence to recommend the routine use of commercially available supplements for treating dry eye syndrome. Vitamin A and Vitamin D might work, but research on their effectiveness is ongoing. It is advisable to consult a doctor before using any supplements for the treatment of dry eyes.
A diet that has adequate good fats may benefit patients with rheumatoid arthritis, both in terms of joint pains and in terms of eye health. Vitamins A and D are fat soluble vitamins. Rather than get these from isolated vitamin pills, including good fats such as butter, ghee and coconut oil in your diet may be a more natural way of getting the right vitamins needed for your eyes.
An inflammation of the white part of the eye (the sclera) is called scleritis. The sclera is the connective tissue that makes up the outer wall of the eye. An inflammation of this tissue can be dangerous, because even minor trauma can cause the affected part of the eyeball to split open.
Scleritis is an indication that inflammation is out of control, not just in the eye, but elsewhere in the body. It’s also a warning sign to keep your arthritis under control.
Your ophthalmologist may prescribe corticosteroid eye drops to control inflammation, but often the problem is too deep within the eye to be controlled locally. Immunosuppressive agents may also be prescribed.
Vitamin A contains antioxidant compounds that are important for promoting healthy vision by reducing inflammation. Vitamin A also helps the cornea (the eye’s surface) to create a barrier for bacteria and viruses, thus decreasing the risk of eye infections.
A case report published in 1998 in the “Canadian Journal of Ophthalmology” described the situation of a patient who developed scleritis due to a vitamin B12 deficiency. Eggs, meat, poultry, shellfish and milk products are some good sources of vitamin B12.
Vitamin C has been shown to relieve the pain and light sensitivity of scleritis more rapidly, and to shorten the duration of the condition than with medicinal treatment alone. Since vitamin C is safe in relatively high doses, taking 2,000-milligram supplements several times a day can be effective in relieving the pain and redness associated with scleritis quickly.
Vitamin D deficiency can cause inflammation, which is why this vitamin is often prescribed to treat and prevent inflammatory diseases like heart disease, multiple sclerosis, rheumatoid arthritis and, potentially, scleritis.
Uvea is the middle part of the eye between the sclera and retina. And iris is the colored part of the eye that helps control the light entering it. An inflammation of the uvea is known as uveitis and that of the iris is called iritis.
If not controlled, uveitis can lead to vision loss.
Keeping your arthritis under control can help to minimize the risk to your eyes, but if you have symptoms of uveitis and iritis, contact your ophthalmologist at the earliest. Usually, the first line of treatment is corticosteroid eye drops. If inflammation is severe, an oral or injectable corticosteroid may be preferred. Doctors may also prescribe antibiotics in case of an infection.
Along with corticosteroids, you can try some supplements to deal with uveitis and iritis. However, there is limited evidence to support their effectiveness.
A pilot study in 32 patients concluded that systemic echinacea appears safe and effective in controlling low-grade autoimmune idiopathic uveitis.
The efficacy of turmeric was found to be comparable to the standard treatment for uveitis in a small subset of patients.
Anecdotal reports suggesting possible effectiveness of vitamin E on uveitis and iritis are available.
Certain types of inflammatory arthritis, such as psoriatic arthritis or an excessive use of corticosteroids to treat arthritis, may lead to early development of cataracts and glaucoma (increased pressure of the eye). Thus, regular visits to the ophthalmologist while on steroid therapy is a must.
To conclude, arthritis can pose serious risks for eye health. If you’re suffering from arthritis, be mindful of your diet and lifestyle to safeguard your eyes and prevent long-term damage to them.