
Menopause
Menopause Hot Flashes: Causes & Natural Treatment
Aug 2, 2019Sheila sits uncomfortable, with sweat beads lining up her brow. She wonders when the others will notice that she is literally burning up. Can they see it? Did it suddenly get hot in here, or is it just her? Just one minute ago, she was perfectly fine, chatting with her colleague in the conference room and now, she wonders if the air conditioner could be cranked up to maximum. Sheila has just met the first sign of menopause.
Menopause can come with symptoms that are difficult to deal with. Hot flashes can often be at the top of the list of these symptoms.
With menopause, women begin to have lower levels of the hormone estrogen. And while science still doesn’t have a definitive answer as to ‘why’ women get hot flashes, they are a common symptom of perimenopause as well as menopause.
Let’s take a closer look at what exactly these hot flashes causes are, and what you can do to reduce the severity of this pesky symptom of menopause.
What Is a Hot Flash?
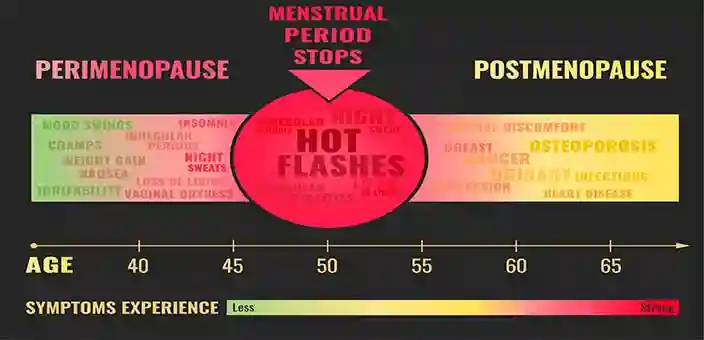
As the name suggests, a hot flash is the sudden onset of intense heat, which is often unrelated to external factors. It’s accompanied by sweat and sometimes a red, flushed face and/or neck too. Sometimes they happen while you’re asleep, and are known as night sweats as well.
Some common symptoms of hot flashes are:
- Face and neck becoming flushed
- Sweating, particularly above the chest
- Chills
- Skin feeling warm, even when it’s not warm outside
- Faster heart beat
- Tingling in fingers
What Causes Hot Flashes?
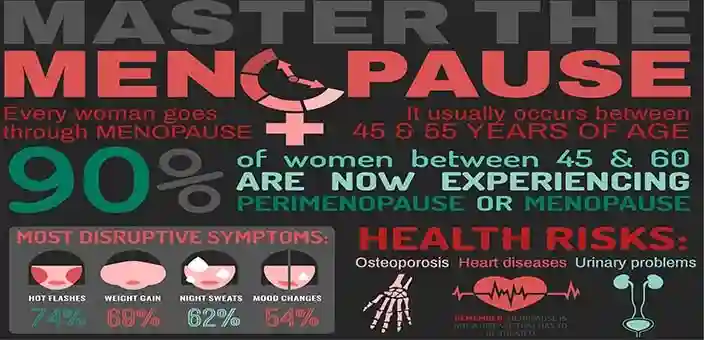
Science has been unable to pinpoint the exact cause behind hot flashes, but they are closely linked to hormonal fluctuations, which is why they’re so common in perimenopause and menopausal women. Changing hormone levels affects circulation, causing blood vessels closest to the skin to widen in an attempt to cool off. This is what causes the flushing and sweating.
Let’s get into the science of it, shall we?
The hypothalamus is the part of the brain that acts as the master control of our body temperature. Think of it as our main temperature control unit. It has a “null” zone which is 0.4 degrees centigrade wide, and the function of this zone is to ensure that small changes in external environment don’t throw off your core body temperature. For example if the temperature raises or drops by a few degrees, this main control unit ensures our body doesn’t resort to extreme reactions – like vasodilation or constriction of arteries and veins – which can cause chills, shivers or profuse sweating.
Around menopause, this thermo-regulatory center seems to go through a fundamental change, leading to a loss of sensitivity to this null zone. This is why even small changes in external factors – like heat, cold, stress, etc. lead to the body having an extreme reaction to try and correct for the external stimulus.
A comprehensive 2014 research paper called Menopausal Hot Flashes: Mechanisms, Endocrinology, Treatment by Robert R. Freedman, Ph.D proposed that this mechanism of loss of sensitivity was caused by hormonal changes that a woman undergoes during menopause. There’s an increase in the levels of the neurotransmitter Norepinephrine (also known as ‘Stress Hormone’) in the hypothalamus, which in turn is caused by lower levels of oestrogen in menopausal women. Together, these hormonal fluctuations lead to a narrowing of the null zone.
Serotonin was proposed to have the ability to reduce the effects of norepinephrine, thereby lowering hot flashes. That is why anti-depressants, that have serotonin like effects, are sometimes prescribed by allopathic doctors to menopausal women, even in the absence of regular depression symptoms.
Who Is Susceptible To Hot Flashes?
Hot Flashes can start suddenly, and are seen in women with menopause and perimenopause as well. Perimenopause is the period before the inset of menopause and can last anywhere from 4 to 7 years, before your periods stop completely.
Sometimes hot flashes are also seen in women who undergo hysterectomy, oophorectomy or chemotherapy, because these medical procedures interfere with your hormones, mainly with oestrogen.
However, some women never get hot flashes, while others can experience them for more than 11 years. Lifestyle factors that affect hormones can sometimes worsen hot flashes. This is why women with metabolic syndrome, diabetes type 2 and those who are obese may experience them more often.
How Long Do Hot Flashes Last?
It’s difficult to define how long hot flashes last. Since they are intrinsically linked to hormonal fluctuations, they vary from one woman to another.
For some women, a hot flash may pass in just a few minutes, while others can have episodes lasting 10 minutes or more. The frequency of hot flashes is also dependent on your individual hormonal fluctuations. Some women can experience several hot flashes in an hour, while others have a few per week.
For some women, hot flashes are nothing but as minor annoyance, while for others, the severity and intensity can negatively affect quality of life.
How long hot flashes last is dependent on how wildly your hormones are fluctuating during perimenopause or menopause, which is why lifestyle changes and modifications that aim to help stabilize hormones are the key to easy transitioning to menopausal life.
What Are Some Common Triggers
Each woman’s hormones have a delicate balance of their own, which is why triggers vary from one woman to the next. However, some common triggers for hot flashes are:
- Stress or Anxiety
- Being in hot temperatures
- Wearing tight, restrictive clothing
- Caffeine intake
- Smoking
- Drinking alcohol
- Eating spicy foods
- Bending over suddenly
It’s a good idea to identify your triggers, as this can help make hot flashes less frequent and/or severe. While it is not possible to prevent hot flashes completely during menopause, avoiding or controlling your triggers will go a long way towards improving your quality of life.
Conventional Treatment And Their Downsides
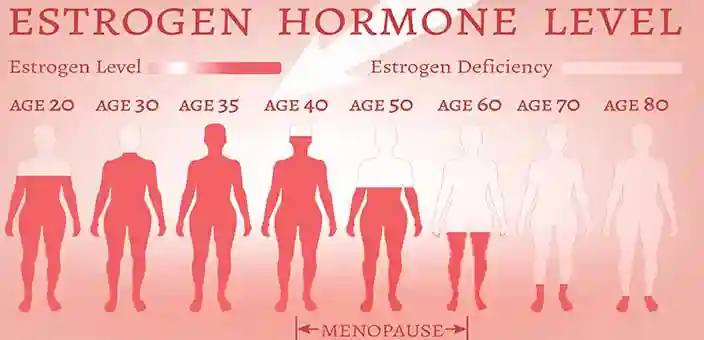
For years, Hormone Replacement Therapy (HRT) was the conventional treatment for all menopause related symptoms, but their popularity has waned in recent times. Many women who tried HRT using synthetic hormones found that their hot flashes and other symptoms returned the minute they stopped using artificial hormones.
HRT cannot be used for women who have had breast/uterine/endometrial cancer in the past. In fact, studies find that HRT could also raise risk of cancer in people without a past history of cancer. And don’t be fooled into thinking that estrogen-only HRT is the only evil. Research finds strong evidence that the addition of a progestin to HRT markedly enhances the risk of breast cancer as well.
However, cancer is not the only downside of HRT. Using artificial hormones to treat symptoms of menopause have also been scientifically linked with increased risk for memory loss and dementia, urinary incontinence, blot clots, incidences of heart attack and stroke, osteoporosis, venous thromboembolic disease, as well as ineffective mammograms for breast-cancer detection.
Bio-identical hormones, derived entirely from plants, have emerged as a strong alternative to synthetic HRT, but people still worry about having to take external hormones due to the association with earlier HRT. All things considered, natural, alternative, safe therapies as well as lifestyle modifications can be a very effective way to treat hot flashes.
6 Natural Solutions To Minimize Hot Flashes
While hot flashes are a part and parcel of life with menopause, there are several steps you can take to reduce their severity and intensity. Alternate therapies and lifestyle modifications don’t just help hot flashes, they also help minimize other annoying symptoms of menopause (like low libido, fatigue, weight gain and more) as you become healthier, fitter and better able to transition to menopausal life.
Practice Mindfulness
Stress releases epinephrine – a hormone that increases core body temperature and causes sweating. Practicing mindfulness using relaxing techniques goes a long way towards decreasing frequency and severity of hot flashes.
Make some “me” time for yourself every day. Sit down and relax with a cup of tea and do things that help calm your mind – be it listening to music, reading a good book or simply enjoying your beautiful garden. Remember, the onset of a hot flash can trigger anxiety, intensifying your symptoms. Calming techniques come very handy to keep stress at bay and make living with menopause a lot easier.
Some relaxing techniques worth trying are:

- Deep breathing exercises
- Yoga
- Meditation
- Acupuncture
- Massage
- Talk therapies with a counsellor or even a close confidant
- Guided thought
Identify Your Triggers
Since triggers for menopause vary from woman to woman, it is worth identifying your personal triggers. And then making conscious efforts to avoid or minimize them.
Here are some tips:
- Quit smoking today. If someone else smokes in your family, avoid exposure to second-hand cigarette smoke as well.
- If you cannot give up drinking completely, it’s wise to cut back as much as possible.
- Avoid wearing tight, form-fitting clothes. Instead, opt for flowy silhouettes that allow better circulation and choose natural fabrics that breathe more easily. Make sure your first layer of clothing is cotton, even in winter.
- If you experience night sweats, it’s a good idea to change bed linen to cotton. While silks and satin fabrics feel soft against the body, these don’t breathe easily, making you more likely to wake up from the sweating.
- If you notice that your hot flashes worsen on a hot day, plan to stay indoors where it’s cooler. Handheld fans do a great job of cooling you off in case you start sweating profusely and can’t get into air-conditioned indoors immediately. You can also carry a bottle of cool water with you at all times. Hydrate when you start to heat up and splash some cold water on your face and neck for some immediate relief.
- Lose weight, as hot flashes are more common in overweight women. Not only will weight loss help improve your health markers; it will also reduce frequency and intensity of hot flashes. Follow a healthier diet and try gentle exercises to drop the weight.
Eat Right

We cannot stress on this enough – you are what you eat. Eating a nutrient-dense, balanced diet that comprises of healthy fats and proteins helps stabilize hormones, which greatly improves all menopause symptoms like hot flashes.
Give up on highly refined, sugar-loaded foods and instead opt for:
Healthy Carbs
Ditch white bread, rice and pasta, and instead opt for healthier carbs like lots of green, fibrous vegetables, fruits and whole grains
Healthy Fats
Choose foods rich in omega-3 fatty acids like fish, seafood, avocado, seeds and nuts. Replace generic refined cooking oils with grass-fed ghee, butter, cold-pressed coconut oil and olive oil, as these healthy fats improve insulin sensitivity, boost heart health and also stabilize hormones.
Healthy Proteins
Opt for lean cuts of meats, eggs, chicken and turkey, fish and seafood and give up on processed meats and cold cuts like bacon, sausages, salamis and fried snacks. Lentils and legumes are other good sources of protein for vegetarians.
Foods to Avoid in Hot Flashes

On the other hand, some foods are known to worsen hot flashes and are best avoided.
Spicy foods
These increase body temperature, triggering hot flashes. Instead, add flavour to your meals with fresh or dried herbs.
Caffeinated beverages
These are common culprits. Switch to herbal or green tea instead.
High-sugar diets and processed foods
Along with trans-fats, these cause weight gain and worsen all symptoms of menopause.
Alcohol
Drinking that beer or wine can increase severity and frequency of hot flashes.
In fact, a study found that eating a Mediterranean style diet, which includes fresh fruits, veggies, whole grains and fish, helped reduce hot flashes.
Moderate Exercise Helps

Not only will exercising regularly help you lose weight, it also helps improve hormone stability. Go for an evening walk, try swimming, take tap dancing lessons or try yoga for fitness.
Alternative Therapies Are Worth Trying
Alternative therapies can also alleviate symptoms of menopause, like hot flashes. In particular, Cognitive Behaviour Therapy (CBT) can help develop practical skills and techniques to manage hot flushes.
Studies have found that CBT is widely applicable for women having problematic hot flashes and night sweats, regardless of sociodemographic or health-related factors, and that CBT works mainly by changing the cognitive appraisal of handling menopausal symptoms.
For some, acupressure, acupuncture and herbal therapies can help reduce hot flashes.
Sepalika Menopause Treatment Program
The Sepalika Menopause Programme is scientifically designed to help women deal with not just hot flashes, but also all the other symptoms of peri-menopause and menopause. Each person’s treatment is tailor-made as per their symptoms, medical history and lab test results. Progress is tracked till you get better and expert supervision is available throughout the programme. Write to us at health@sepalika.com for more information and to speak to a Health Coach today! Note: This program is open to women living in India only.
This article has been co-authored by Maneera Saxena Behl, a health and fitness who likes to help others improve their overall well-being by achieving the right balance between nutrition, exercise and mindfulness.
References:
References:
Use of HRT and the subsequent risk of cancer – https://europepmc.org/abstract/med/10695959
Effect of Hormone Replacement Therapy on Breast Cancer Risk: Estrogen Versus Estrogen Plus Progestin – https://academic.oup.com/jnci/article/92/4/328/2624742
Hormone replacement therapy (HRT)— risks and benefits – https://academic.oup.com/ije/article/30/3/423/736896
Fruit, Mediterranean-style, and high-fat and -sugar diets are associated with the risk of night sweats and hot flushes in midlife: results from a prospective cohort study – https://academic.oup.com/ajcn/article/97/5/1092/4577089
Cognitive-behavior therapy for menopausal symptoms (hot flushes and night sweats): moderators and mediators of treatment effects – https://www.ncbi.nlm.nih.gov/pubmed/24149919
MENOPAUSAL HOT FLASHES: MECHANISMS, ENDOCRINOLOGY, TREATMENT – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4612529/#R55



